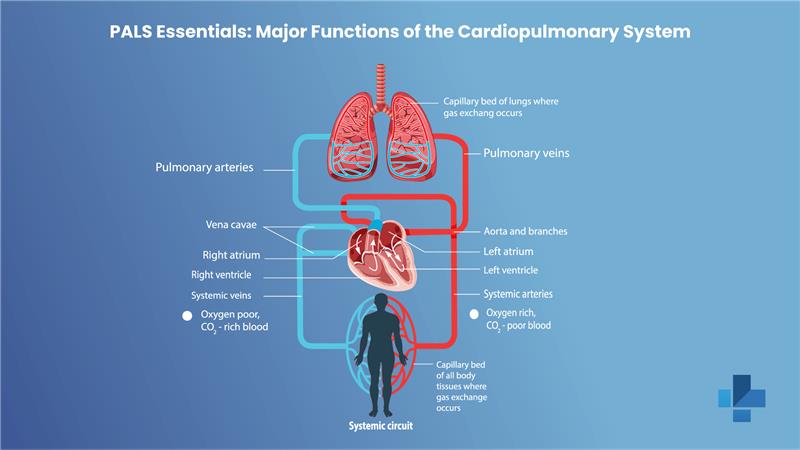
Success in Pediatric Advanced Life Support (PALS) depends on understanding how a child’s heart and lungs work together to deliver oxygen to the body, specifically during illness or cardiac or respiratory emergencies. The PALS cardiopulmonary system is designed to maintain oxygen delivery, remove metabolic waste, and ensure adequate circulation to vital organs.
Because children have different pediatric cardiopulmonary physiology as compared with adults, recognizing how these systems function under stress is critical for early intervention. Before pursuing PALS certification, healthcare professionals should master 4 fundamental cardiopulmonary functions that determine how effectively oxygen is delivered throughout the body.
Function 1: Oxygenation
The first critical function of the PALS cardiopulmonary system is oxygenation, the process by which oxygen enters the bloodstream through the lungs. During breathing, air travels through the airway and reaches the alveoli, where oxygen diffuses into the pulmonary capillaries. Adequate oxygenation ensures that oxygen binds to hemoglobin and is transported throughout the body.
In PALS oxygenation lungs physiology, children are more vulnerable to oxygenation problems because:
- Their airways are smaller and more easily obstructed
- Oxygen reserves are lower than in adults
- Oxygen consumption is higher relative to body size
Because of these factors, pediatric patients can deteriorate quickly when oxygenation is compromised. Early signs such as increased respiratory effort, nasal flaring, or decreased oxygen saturation require immediate evaluation and support.
Function 2: Carbon Dioxide Removal
The second major role of the cardiopulmonary system is ventilation, the removal of carbon dioxide (CO₂) from the body.
In PALS ventilation CO₂ physiology, CO₂ produced during cellular metabolism travels through the bloodstream to the lungs. During exhalation, it is expelled from the body. When ventilation becomes inadequate, CO₂ accumulates in the bloodstream, which can lead to respiratory acidosis and worsening clinical instability.
In pediatric emergencies, common causes of impaired ventilation include:
- Airway obstruction
- Respiratory muscle fatigue
- Severe lung disease
- Depressed respiratory drive
It is critical to monitor ventilation during resuscitation. End-tidal CO₂ monitoring provides real-time information about ventilation efficiency and helps to guide treatment decisions during advanced life support.
Function 3: Pressure Generation
The third critical function involves the heart’s ability to generate pressure to circulate blood effectively.
In the PALS cardiac output pressure model, cardiac output is determined by two major factors:
- Heart rate
- Stroke volume
Unlike adults, children rely heavily on heart rate to maintain cardiac output because their hearts have a limited ability to increase stroke volume. This means that bradycardia (slow heart rate) can quickly lead to poor circulation and cardiovascular collapse.
Pressure generation ensures that oxygenated blood moves from the heart to the lungs and then to the rest of the body. If the heart cannot generate sufficient pressure, tissues receive inadequate oxygen despite normal lung function. This is why PALS algorithms emphasize rapid recognition and treatment of pediatric bradycardia and shock.
Function 4: Systemic Perfusion
The final function of the cardiopulmonary system is systemic perfusion, the delivery of oxygenated blood to tissues and organs. The PALS circulation perfusion process ensures that vital organs like the brain, heart, and kidneys receive the oxygen and nutrients needed to function properly.
When perfusion is impaired, tissues become hypoxic, and organ dysfunction can develop rapidly. Signs of poor perfusion in children include:
- Altered mental status
- Delayed capillary refill
- Cool or mottled skin
- Weak pulses
- Low blood pressure (a late sign in pediatric shock)
Recognizing early indicators of impaired perfusion allows clinicians to intervene before cardiac arrest occurs.
PALS Integration
Understanding these four functions: oxygenation, ventilation, pressure generation, and perfusion is essential for accurate PALS cardiopulmonary assessment during pediatric emergencies.
In PALS training, these functions are integrated into rapid clinical evaluation tools like the Pediatric Assessment Triangle (PAT), which helps providers quickly determine whether a child is experiencing respiratory distress, respiratory failure, or circulatory compromise. By systematically evaluating airway, breathing, and circulation, clinicians can identify which cardiopulmonary function is failing and intervene appropriately.
For a complete overview of PALS training requirements, see the PALS Certification Guide.
medtigo PALS Mastery
Learning pediatric cardiopulmonary physiology is easier when combined with hands-on practice and scenario-based training. With medtigo PALS training, healthcare professionals can practice recognizing cardiopulmonary dysfunction and responding effectively during pediatric emergencies.
Interactive learning modules allow you to:
- Apply PALS algorithms in simulated cases
- Strengthen pediatric assessment skills
- Improve decision-making during critical scenarios
Practice these functions in interactive modules and build confidence before certification.
Master PALS Cardiopulmonary Online – Enroll today!
FAQs
1. Why is heart rate higher in determining cardiac output in children?
Children rely more on heart rate to maintain cardiac output because their hearts have a limited ability to increase stroke volume. As a result, decreases in heart rate can rapidly reduce cardiac output and compromise circulation.
2. What is the normal EtCO₂ range in PALS?
The normal end-tidal carbon dioxide (EtCO₂) range during effective ventilation is typically 35 to 45 mmHg. During CPR, maintaining EtCO₂ levels above 10 to 20 mmHg indicates adequate chest compressions and perfusion.















