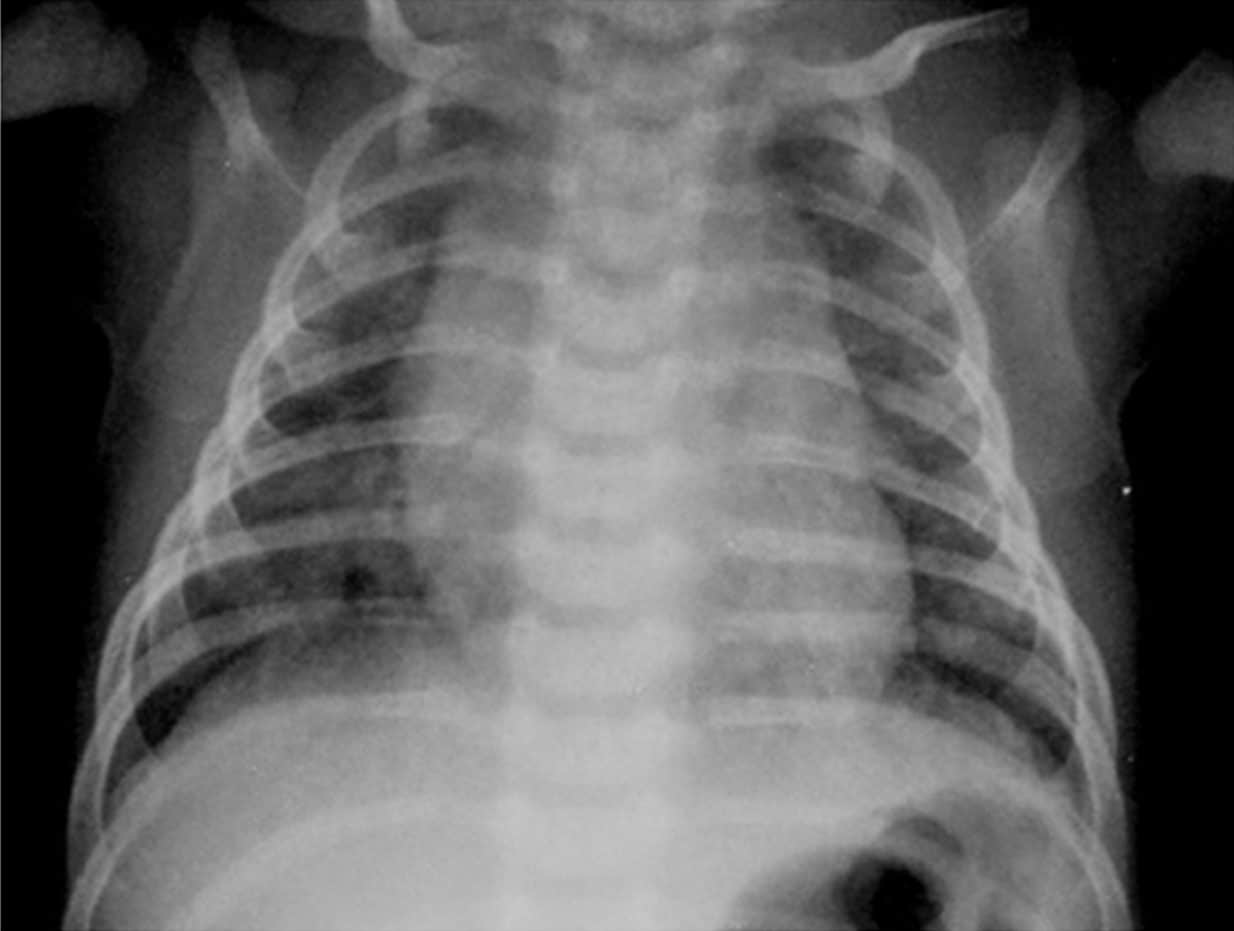
Skin cancer — the abnormal growth of skin cells — most often develops on skin exposed to the sun.
But this common form of cancer can also occur on areas of your skin not ordinarily exposed to sunlight.
There are three major types of skin cancer — basal cell carcinoma, squamous cell carcinoma and melanoma.

Melanoma is a malignant melanocyte tumor. Melanocytes are the cells that produce the pigment melanin and are generated from the neural crest. While most melanomas begin on the skin, they can also develop on mucosal surfaces or in other locations where neural crest cells migrate.
The global incidence of malignant melanoma is increasing at a higher rate than that of any other cancer. Melanoma is more common in white people than in black people and Asian people. The average age upon diagnosis is 57 years, and up to 75% of patients are under the age of 70

Independent nurse
Melanomas can grow in or near a precancerous lesion or otherwise seemingly healthy skin. Melanomas which develop in healthy skin arise de novo, without any signs of precursor lesions. Solar exposure is the most common risk factor for melanomas.
Other risk factors include pre-existing nape us, Family history, Higher age, and more than 50 moles of 2mm or more in diameter. Melanoma can also develop in parts of the skin that are not exposed to the sun, such as the palms, soles, and perineum.
Certain lesions are regarded as precursors to melanoma. Among these are nevi such as Common acquired nevus, Dysplastic nevus, Congenital nevus Cellular blue nevus Melanomas grow in two distinct stages: radial and vertical

Medscape
Changes in the size, shape, color, or feel of a mole are often the first warning signs of melanoma.
These changes can occur in an existing mole, or melanoma may appear as a new or unusual-looking mole.
The “ABCDE” rule is helpful in remembering the warning signs of melanoma:
Types of Melanoma
The 4 most common types of skin, or cutaneous, melanoma are:

Doctors use many tests to find or diagnose cancer. They also do tests to learn if cancer has spread to another part of the body from where it started. If this happens, it is called metastasis. For melanoma, a excisional biopsy of the suspicious skin area, called a lesion, is the only sure way for the doctor to know if it is cancer.
In a biopsy, the doctor takes a small sample of tissue for testing in a laboratory. The doctor may suggest other tests that will help make a diagnosis and determine the overall stage of the melanoma.
The doctor may also look out for the thickness of tumor. The thickness of the primary melanoma tumor is the most reliable characteristic that helps doctors predict the risk that cancer will spread.
To do this, the pathologist will measure the depth of the melanoma from near the top of the skin down to the bottom of the melanoma in the underlying skin or fatty tissue below.
Sentinel lymph node biopsy — also called SLNB, sentinel node biopsy, or SNB—is a surgical procedure that helps the doctor find out whether the cancer has spread to the lymph nodes.

Stratum dermatology clinic
The main treatment for melanoma is surgical removal, or excision, of the primary melanoma on the skin. The extent of the surgery depends on the thickness of the melanoma. Most melanomas are found when they are less than 1.0 mm thick, and outpatient surgery is often the only treatment needed.
A doctor removes the tumor, the tissue found under the skin, and some surrounding healthy tissue, called a margin so that no cancer cells remain. If a sentinel lymph node biopsy is also needed, it is usually done at the same time as the wide excision.
Margins are to be removed as well, along with the primary lesion. The area of margin to be removed depends on the area of the primary lesion or its depth of it.
Some immunotherapy drugs are relevant nowadays like –
Basal cell Carcinoma

Basal Cell Carcinoma is the most common type of human cancer worldwide, and it is a subtype of non-melanoma skin cancer that is on the rise due to an aging population and widespread sun exposure. Basal Cell Carcinoma has a growing incidence rate worldwide, and it is more common in areas with increased UV exposure, such as those at higher or lower latitudes.
A history of squamous cell carcinoma or BCC is the most common predictor of BCC development. Patients with a history of Basal Cell Carcinoma are at least 10 times more likely to acquire a second BCC diagnosis than patients without a history of non-melanoma skin cancer. Estimated incidence rates have climbed between 20%-80% in the last 30 years. Men are more likely than women to develop this cancer.

BCC etiology is determined by the interaction of the patient’s environmental and genetic features. The pathophysiology of this disease is through to be caused by an abnormal stimulation of the Hedgehog signalling system.
Direct DNA damage, indirect DNA damage via reactive oxygen species, and immunological suppression are the mechanisms of BCC formations caused by UV exposure. Melanin absorbs UVA rays, due to which the DNA experiences free radical damage.
UVB exposure directly damages DNA and RNA by causing a change in CC/TT or C/T. UV radiation also suppresses the cutaneous immune system in a dose-dependant manner, compromising immunological monitoring of skin cancer.

There are numerous clinical forms of basal cell carcinoma (BCC). However, the most common types of Basal Cell carcinoma are superficial, nodular, and morphea form. The majority of BCCs are nodular.
Mostly, BCC is characterized by pink or flesh-colored nodules or papule with telangiectasia. The tumor may enlarge and ulcerate, giving the borders a rolled or rodent ulcer appearance.
Nodular Basal cells are most commonly found on the face, specifically on the cheeks, nasolabial folds, eyelids, and the forehead. The trunk and limbs are low-risk locations, whereas the cheeks, forehead, neck, scalp, and chin present an intermediate risk of recurrence.
Anatomical regions such as the nose, ears, centrofacial, and periorificial areas are high-risk locations. Morpheaform BCCs are typically white or flesh-colored with patches of induration and a borderless appearance.

EWFB57
A skin sample is required for confirmation of basal cell carcinoma. Shave, punch, and excisional biopsies are all viable alternatives. Shave and punch biopsies are only around 80% accurate for diagnosing the multiple subtypes of BCC.
Preoperative imaging studies are suggested when there are indications of muscle, deep soft tissue, parotid glad, bone involvement, or perineural invasion. Clinicians with experience can use dermoscopy to aid in the identification of nonpigmented and pigmented basal cell carcinomas.
On dermoscopy, BCC is distinguished by the presence of well-focused, arborizing vessels. Patients having a history of BCC, especially those with many tumors or high-risk tumors should have long term, or preferably life-time follow-ups.

Everyday health
In most cases, BCC is treated surgically. However, other kinds are responsive to medicinal or radiation therapy.
The suggested methods of therapy used to treat Basal Cell Carcinoma are:
● Surgical excisions
● Radiation therapy
● Hedgehog pathway inhibitors
● Photodynamic therapy
● Cryosurgery
● Topical therapies
Mohs surgery has the highest long-term cure percentage of any therapy technique for basal cell carcinoma. It is the treatment of choice due to its tissue sparing effect.
Squamous Cell carcinoma
Radiation therapy is the primary treatment option for BCC and SCC when surgery is contraindicated. It can also be utilized as a treatment following surgery when additional surgery will jeopardize major nerves or other critical structures or when cancer cells have invaded the perineural space.
Sonidegib is another Hedgehog pathway inhibitor such as Vismodegib is prescribed. 55% of patients discontinue these medications due to severe physical side-effects.

In the United States, squamous cell carcinoma of the skin, also known as cutaneous squamous cell carcinoma, is the second most prevalent form of skin cancer, right behind basal cell carcinoma. Actinic Keratosis appears as a precursor lesion before SCC development; it demonstrates tumor growth and has the ability to spread inside the body.
Ultraviolet (UV) sun radiation is the key risk factor for the development of cutaneous squamous cell carcinoma, and cumulative lifetime exposure plays a significant role in the progression of this malignancy.
Following Basal Cell Carcinoma, SCC is the skin cancer which most people in the US are afflicted with. Previously BCC would affect 3 times more individuals than Squamous Cell Carcinoma, but now the number of individuals affected are almost the same.
They’re both responsible for around 1 million cases each annually. It has been observed that the ratio tends toward the occurrence of squamous cell carcinoma as age increases. White-skinned individuals with light eyes and significant exposure to UV rays are extremely susceptible to SCC, especially after turning 50.

BSIP/Universal Images Group via Getty Images
The leading cause of SCC is solar UV radiation. Squamous cell carcinoma can also be caused by extended periods of exposure to substances which increase cancer risk, such as the tar in cigarettes. Other probable reasons include a severe burn scar, a long-standing ulcer or sore, and some forms of HPV, particularly in the vaginal area.
Some of the common risk factors for Squamous Cell Carcinoma development include tanning lamp usage, exposure to ionizing radiation, and therapeutic exposure to UV rays. These factors probably lead to changes in the p53 pathway.
The p53 protein is responsible for preventing the replication of cells with mutated or damaged DNA. If the p53 gene becomes altered in any of the aforementioned ways, the p53 protein becomes inactive, and cells with damaged DNA, such as those present in squamous cell carcinoma, are able to proliferate.

Medicine net
Most frequently SCC develops through actinic keratoses in individuals with skin damage due to chronic sun exposure. Common sites on which Squamous Cell Carcinoma develops include the shins, extensor forearms, scalp, neck, and face. Variable degrees of scaling, crusting, ulceration, and hyperkeratosis are present, along with varying degrees of flesh-toned to erythematous color.
In some cases, squamous cell carcinoma can be flat, nodular, or even structured like a plaque, with palpable induration which may or may not be accompanied with subcutaneous spread. Sometimes, SCC can be painful and uncomfortable, which could be a sign of perineural invasion.

JAAD CASE REPORTS
Every patient suspected with squamous cell carcinoma must undergo a skin biopsy. On histopathological evaluation, SCC is characterized by irregular cords, nests, and sheets of invading neoplastic keratinocytes.
When predicting the probability of metastasis, thickness of the lesion plays a key role in SCC prognosis, with thicknesses greater than 4 mm being associated with an increased risk.
In instances where the diagnosis is uncertain, it’s suggested to perform immunoperoxidase staining for cytokeratins 5/6/AE1/AE3, particularly in cases of poorly differentiated SCC.

The most preferred treatment for SCC is surgery. Like it is for BCC, the therapy of choice is Mohs surgery. Mohs Surgery is also the preferred treatment for squamous cell carcinoma in immunocompromised individuals, recurring squamous cell carcinoma, and SCC with aggressive histologic characteristics, and squamous cell carcinoma with a depth of at least 2 mm.
Topical or oral retinoids are among other treatments which can lower the risk of SCC formation. In addition to photodynamic theory, topical 5-fluorouracil or imiquimods are used to inhibit the development of SCC. Using a combination of electrodesiccation with curettage or the standard topical treatments such as imiquimods is an effective method of treating the disease.
Patients suffering from cutaneous squamous cell carcinoma must be counselled about skin protection from UV rays. They should use sunscreen, wear protective clothing, and avoid the sun during time periods when it’s at its maximal intensity. Regular follow-ups are also recommended (6-12 months for most cases, and more regularly for aggressive tumors)

Both our subscription plans include Free CME/CPD AMA PRA Category 1 credits.

On course completion, you will receive a full-sized presentation quality digital certificate.
A dynamic medical simulation platform designed to train healthcare professionals and students to effectively run code situations through an immersive hands-on experience in a live, interactive 3D environment.
When you have your licenses, certificates and CMEs in one place, it's easier to track your career growth. You can easily share these with hospitals as well, using your medtigo app.